Abstract
Objective
We studied whether a simple educational intervention would increase patient completion of advance directives and discussions on end-of-life issues.
Design
Randomized, controlled trial.
Setting
Outpatient clinic of a teaching hospital.
Subjects
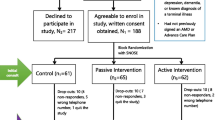
One hundred eighty-seven outpatients of a primary care internal medicine clinic.
Intervention
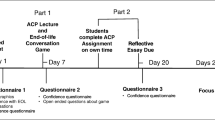
Study subjects attended a 1-hour interactive seminar and received an informational pamphlet and advance directive forms. Control subjects received by mail the pamphlet and forms only.
Measurements and main results
Completion of the advance directive was the main measurement. There were no significant differences in baseline characteristics of either group. Follow-up at 1 month revealed advance directive completion in 38% of study versus 24% of control subjects (p=.04), and discussions on advance planning in 73% of study versus 57% of control subjects (p=.02). Patients most likely to complete the documents were white, married, or attendees at the educational seminar.
Conclusions
Interactive group seminars for medical outpatients increased discussions and use of written advance directives.
Similar content being viewed by others
References
Annas GJ, Arnold B, Aroskar M, et al. Bioethicists' statement on the U.S. supreme court's Cruzan decision. N Engl J Med. 1990; 323:686–7.
Emmanuel EJ, Weinberg DS, Gonin R, Hummel LR, Emmanuel LL. How well is the patient self-determination act working? An early assessment. Am J Med. 1993;95:619–28.
Hare J, Nelson C. Will outpatients complete living wills? A comparison of two interventions. J Gen Intern Med. 1991;6:41–6.
Teno J, Fleishman J, Brock DW, et al. The use of formal prior directives among patients with HIV-related diseases. J Gen Intern Med. 1990;5:490–4.
Johnson JE, Pinholt EM, Jenkins TR, Carpenter JL. Content of ambulatory internal medicine practice in an academic Army medical center and an Army community hospital. Mil Med. 1988; 153:21–5.
Right to Die: The Choice is Yours [videotape]. New York, NY: Society for the Right to Die; 1988.
Choice in dying. In: About Advance Medical Directives. South Deerfield, Mass: Channing L. Bete Co.: 1991.
Cox DM, Sachs GA. Advance directives and the patient self-determination act. Clin Geriatr Med. 1994;10:431–43.
Emmanuel L. Advance directives: what have we learned so far? J Clin Ethics. 1993;4:8–15.
Rubin SM, Strull WM, Fialkow MF, Weiss SJ, Lo B. Increasing the completion of the durable power of attorney for health care. A randomized, controlled trial. JAMA. 1994;271:209–12.
Sachs G, Stocking C, Miles S. Empowerment of the older patient? A randomized, controlled trial to increase discussion and use of advance directives. J Am Geriatr Soc. 1992;40:269–73.
Cox DM, Sachs GA. Advance directives and the patient self-determination act. Clin Ethics. 1994;10:431–43.
Stelter KL, Elliot BA, Bruno CA. Living will completion in older adults. Arch Intern Med. 1992;152:954–9.
Morrison RS, Olson E, Mertz KR, Meier DE. The inaccessibility of advance directives on transfer from ambulatory to acute care settings. JAMA. 1995;274:478–82.
Author information
Authors and Affiliations
Additional information
Supported by the Department of Clinical Investigations, Walter Reed Army Medical Center.
The opinions or assertions contained herein are the private views of the authors and are not to be construed as reflecting the views of the Department of the Army or the Department of Defense.
Rights and permissions
About this article
Cite this article
Landry, F.J., Kroenke, K., Lucas, C. et al. Increasing the use of advance directives in medical outpatients. J GEN INTERN MED 12, 412–415 (1997). https://doi.org/10.1046/j.1525-1497.1997.00072.x
Issue Date:
DOI: https://doi.org/10.1046/j.1525-1497.1997.00072.x